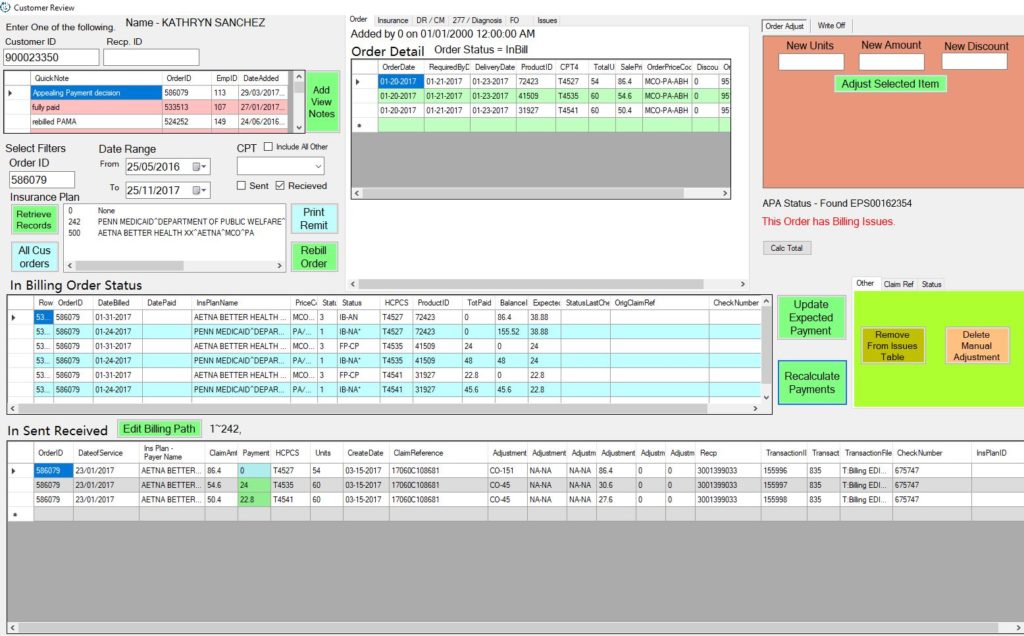
BILLING ORDER STATUSES
Fully paid complete – When you see FP-CP that means that line item or order has fully reached its payment amount (paid in full). There is NO ACTION that needs to be done to that line item or order.
Partially Paid complete – When you see PP-CP that means the insurance companies paid their allowable amount. In most cases, any payment that is left is probably a copay and is owed by the consumer.
Partially Paid Attention needed – When you see PP-AN that means that you received a response from the insurance company but it wasn’t paid to the fee schedule set price. Which means the biller should identify which insurance this is because every insurance have different rules & set up. You may have to give that insurance company a call to see what the issue is. For Pennsylvania Medicaid a status of PP-AN can mean two different things, the consumer has another supplier & a return wasn’t done on a previous order and we sent out a replacement order. If the consumer has another supplier the biller should give DPW a call to see if that line item or order was billed by another supplier.
Billers should get the date the other supplier billed & contact a CSR so that products can be stopped from going out on the next order. The CSR will do their part by calling the consumer and making them aware of this issue. If a return wasn’t done on a previous order and we sent out a replacement order the biller should do the following steps contact the CSR that does the returns and let them know that a return wasn’t done & that you need one put in so that you cam either order, *Always read notes they can help you as well*. The way you can identify the issues that were mentions for Pennsylvania Medicaid is by seeing an adjustment code of CO-119 or procedures limited to 4 per calendar month, procedures limited to 300 per 30 days, procedures limited to 300 per month, procedures limited to 2 per 30 days & underpads limited to 180 per 90 days when you are working the paper remittance advice. Don’t just re-bill the order actually see what is causing the status to say PP-AN.
No Payment Attention Needed – When you see NP-AN that means no payment was made to this order, billers need to do the following step before they should try to re bill the order. The biller should check the denial reason &/ or the adjustment reason on the claim. If you don’t understand the denial reason or the adjustment reason follow up with the insurance companies this could be in a form of calling, using their online web portals or Navinet. By following up with the insurance companies they can go more in dept with why that order or line item was denied & if could be easy fix on our end. The way you can identify a no payment attention needed the denial reason or adjustment reason will have a PI-16 along with another reason such as N30. Pay more attention to the secondary adjustment reason.
Initial Billing Attention Needed – When you see IB-AN that means something when wrong with billing, depending on how long that line item or order reflected that status, there is a possible chance that line item or order was never billed. Billers should follow up with the insurance companies to make sure a claim was received it could be in a form of calling. Using their online web portals or Navinet. If a claim was never made it to the insurance company marked the line item or order as RB-NW.
Over Payment Attention needed – When you see OP-AN that doesn’t necessarily mean that order is over paid. The only way you can tell if a line item or order is over paid is by looking at the response you’ve gotten from the insurance company. Some orders you may need to just hit the recalculate payment button and the line items will turn to FP-CP or PP-CP. There are cases where you will see two responses from insurances one will be handed keyed in by a biller & the other will be a computer generated response given to us by a 835 file. The computer generated response will always have a transaction file listed next to each response brought in by a 835 file (example: T:Billing EDI835ReportsPenna835R24C2665-352HHQKL.835). A handed keyed response will have N/A listed as the transaction file. This let you know that we are getting an electronic 835 files back from the insurance company and the billers should stop hand keying in responses. Another case you will see is a double response from the electronic 835 file, if you see two responses that has the same check number, transaction file info & the same payment nlet Mike know he can remove one of the response so that the order can say the correct amount & you recalculate the payment.
Initial Billing Wait – When you see IB-WT that means the computer is waiting for a response from the insurance company. But beware of the time frame the line item or order is resting on IB-WT, because there could be an issue. I usually give the status IB-WT an estimated time frame of three to four months after the claim or 837 file was sent before I start questioning the whereabouts of a response for a HMO/ Medigap/ Medicare replacement plan, Medicaid plans has an estimate time frame of a month & a half, the Medicaid plans are pretty quick with a response of they denied a claim. Typically you will receive a payment response four to five weeks after the insurance had processed the claim.
Denied Suggestive Write off – When you see DN-SWO it means that order or line item was denied & a suggestive write off was made, there is nothing more that is need to be to that order or line item.
Initial Billing Return – When you see IB-RT that means the products on this order was return back to MSI. If a product is return back to MSI that means we can’t bill for it. We have to adjust the items of the order. Billers should make sure the return items wasn’t billed to Medicaid or the MCO for payment, you may had to do an adjustment or void to the order depending on situation.
Initial Billing Attention Needed – When you see the status IB-NA* don’t anything with this status, it is marked that way so that the computer won’t bill that line item.
Initial Billing Item Return – When you see the status IB-ItemRet this means part of this product was return to MSI. Billers should highlight that line item and press the updated expected payment button & the recalculate payments button. If this was a partial return, billers should either RB-NW this order if it is not over the 6 month time frame (Medicaid) or RB-Go the order so that it can be re billed with a product that was already paid. If you don’t know which one to choose, ask a supervisor or a manager.
Fully Paid Complete All – When you see the status FP-CPA this means the computer has looked at all the insurance and found the good denial and the correct payment for the entire order. There is nothing that needs to be done because “ALL” response are in the system.
- RB-NW
- Medicaid – less than 6 month, if with CRN, delete the CRN then send as new claim
- Medicare – we can send the claim as new within 1 year
- RB-GP – more than 6 months claim, attached the CRN of the paid T codes then hit void and adjust
- RB-NEW – Hit the rebill order button then send claim as new
- RB-GO – Hit the rebill order button then send claim as void and adjust
PA WEBSITE
- Gloves are 9 months old
- CO-29 denials
- Claim that has a N286 denial
- In checking customer’s eligibility